Life After a Stent: How to Enjoy Your Summer Vacation Worry-Free
Table of Contents
- Introduction
- 1. Timing is Everything: When Can You Travel?
- 2. Packing for Peace of Mind
- 3. Navigating the Airport Safely
- 4. Beating the Summer Heat
- FAQs
Book a Consultation
Prevention is better than cure. Talk to our specialists today.
Hearing that you need a heart stent can be an overwhelming experience. It is completely normal to feel a mix of relief that the problem was fixed, and anxiety about what comes next.You might find yourself wondering, “Will my life ever go back to normal? Can I still travel and enjoy my summer holidays with my family?”
As an Interventional Cardiologist, I hear these questions all the time. I want to reassure you: the whole point of placing a stent is not to limit your life, but to give your life back to you. A stent is designed to open up a blocked artery, improve blood flow to your heart, and allow you to return to the activities you love.
With summer approaching, you are probably dreaming of a much-needed vacation. Whether you are planning a long train journey, a flight across the country, or a simple weekend getaway, you absolutely can travel after a stent procedure. You just need a little bit of planning.
Here is your simple, worry-free guide to traveling safely this summer.
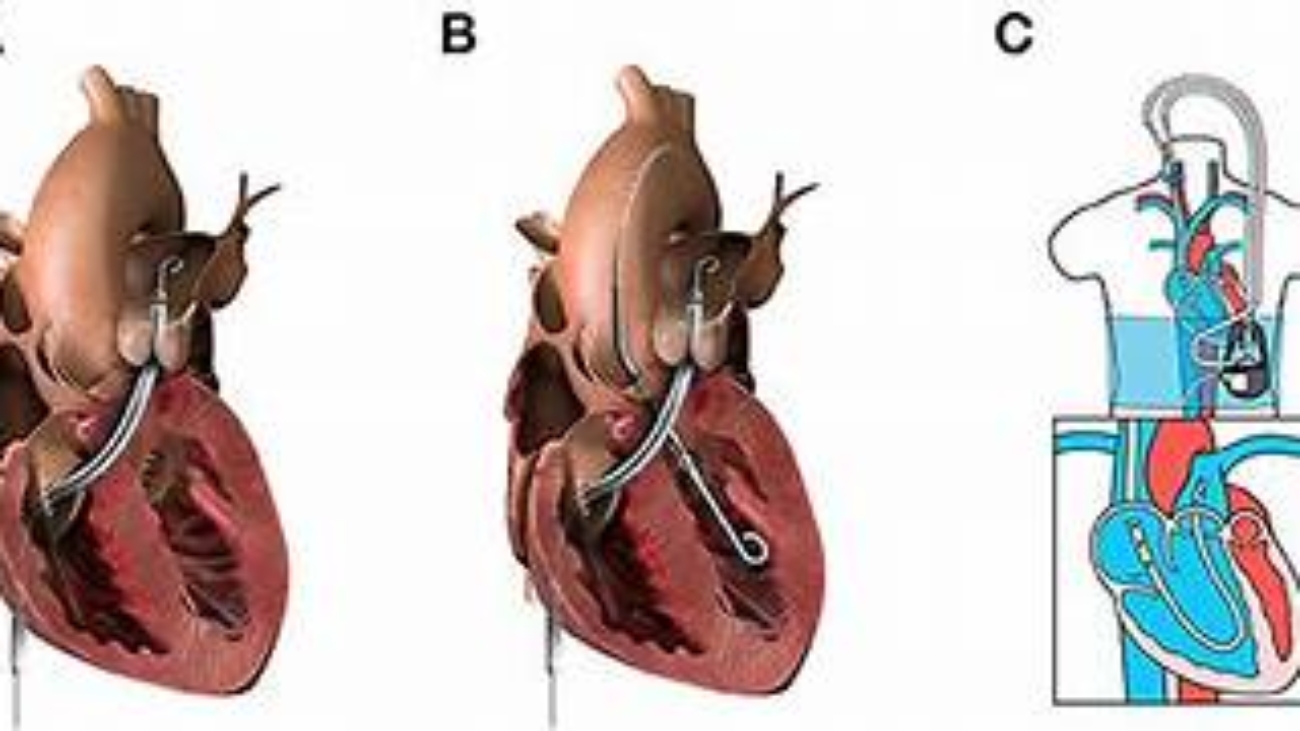
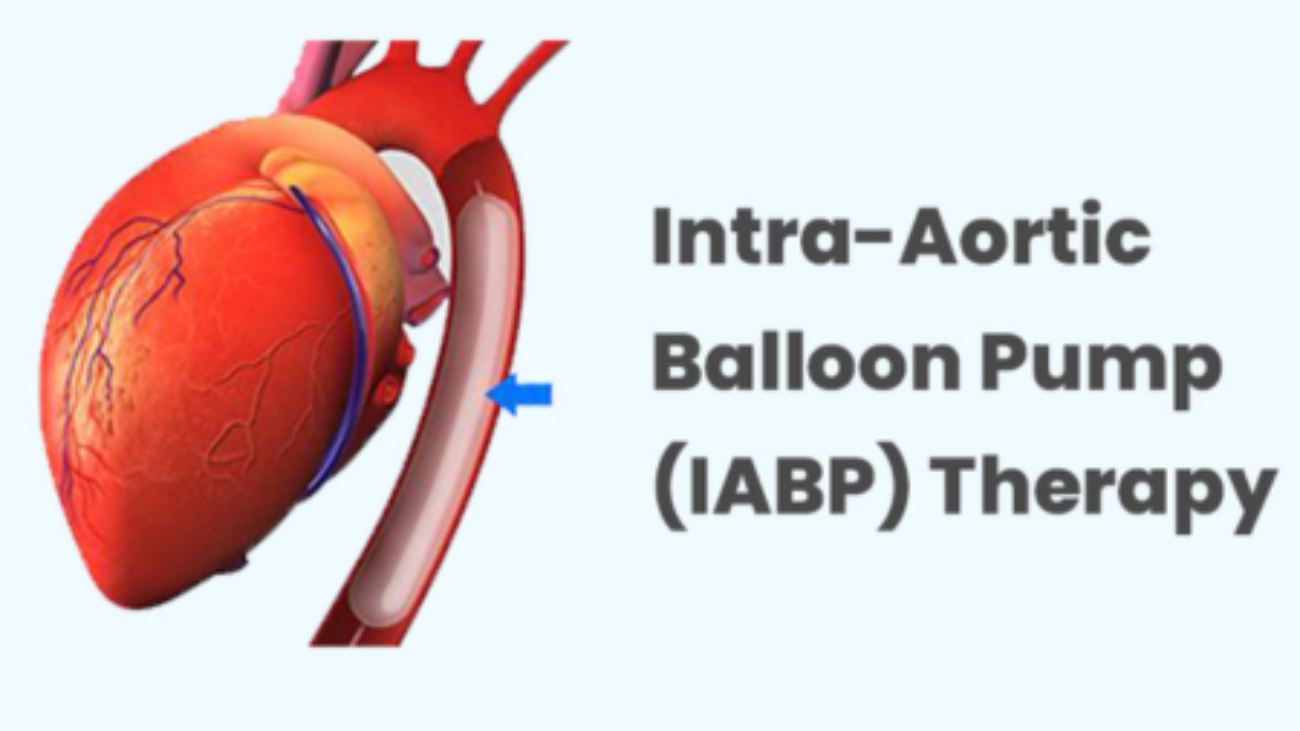
Understanding Your Stent
First, it helps to understand what is happening inside your heart right now. A stent is a tiny, expandable mesh tube.
Once it is placed inside your blocked artery, it acts like a strong scaffold, holding the walls of the artery open so blood can flow freely. Over time, your artery heals over the stent, making it a permanent part of your body. Because the blood is flowing smoothly again, your heart is actually much safer now than it was before the procedure!
1. Timing is Everything: When Can You Travel?
The biggest question is usually when it is safe to pack your bags.
If you had a planned, non-emergency stent procedure and you are feeling well, you might be cleared to travel within a week or two. However, if your stent was placed during a heart attack or a medical emergency, your heart will need more time to rest and heal. In those cases, we usually recommend waiting four to six weeks before taking a big trip.
Always schedule a quick check-up before you confirm your bookings. A simple conversation with your doctor will give you the green light and the peace of mind you need.
2. Packing for Peace of Mind
When packing your suitcase, your heart health should get priority space.
● Double Your Meds: Pack twice the amount of medication you think you will need, just in case your return is delayed. Never pack your essential heart medicines in checked luggage; always keep them in your carry-on bag so they are with you at all times.
● Carry Your Medical ID: Keep a physical copy of your recent ECG, your discharge summary, and your “stent card” (the little card that shows what kind of stent you have).
● Emergency Contacts: Save your doctor’s phone number and the address of a good hospital near your vacation destination in your phone.
3. Navigating the Airport Safely
Many patients worry about airport security. “Will my heart stent set off the metal detectors?” The answer is no. Heart stents are made of non-magnetic metals that will not trigger airport security alarms. You can walk through scanners completely normally.
If you are taking a long flight or train ride, sitting still for hours can increase the risk of blood clots in your legs. Make sure to wear comfortable, loose clothing. Try to stand up, stretch, and walk down the aisle every hour. While sitting, you can also rotate your ankles and wiggle your toes to keep the blood moving.
4. Beating the Summer Heat
Summer vacations usually mean sun and outdoor activities. Remember that extreme heat forces your heart to work harder to cool your body down.
●Stay Hydrated: Drink plenty of water throughout the day. If your doctor has put you on fluid restrictions (which is common for some heart conditions), follow their exact advice on how much you can drink.
● Pace Yourself: You are on vacation, not in a race! Take frequent breaks in the shade or in air-conditioned rooms.
● Avoid the Midday Sun: Plan your sightseeing for the early mornings or lateafternoons when the sun is less harsh.
Listen to Your Heart
The most important rule for traveling after a stent is to listen to your body. If you feel unusually tired, short of breath, or experience any chest discomfort, do not ignore it. Sit down, rest, and seek medical help if the feeling does not go away.
Your heart has been given a fresh start. With your doctor’s approval and a little preparation, there is no reason you cannot enjoy a beautiful, relaxing summer vacation.
Frequently Asked Questions (FAQs)
Expert Care
Hyderabad's leading Cardio & Neuro specialists.